During the Western Regional International Health Conference I had the privilege of lunching with a group of inspirational and innovative undergraduate students from the University of Washington and University of British Columbia. At University of Washington students have created the Critical Development Forum (CDF), a think-tank creating Continue reading
Category Archives: Global Health Education
CFHI Sexual Health in Ecuador Program Highlights Constitutional Priorities
In 1998 Ecuador was the first Latin American country to name reproductive and sexual health as constitutionally guaranteed human rights. Continue reading
Celebrating 20 Years of CFHI
Happy Birthday, Child Family Health International!
2012 marks the 20th anniversary of CFHI’ s transformative Global Health Education Programs and Community Empowerment. This milestone gives us a chance to celebrate and to look back on the impact of CFHI. Continue reading
World AIDS Day 2011
 On this 30th anniversary, World AIDS Day gives us a time to pause and take in the enormity of this disease that has ravaged so much of humanity. There will be much written today about how we are turning a corner and that the epidemic is showing signs of coming to an end. It is important to celebrate and salute the great accomplishments in the fight against AIDS but it is also important to note that we are a long way from taking a victory lap. We do need to build momentum in the fight, so the accolades are helpful as long as they help generate enough buzz and enough energy to follow through by implementing and building on the advancements that have been made.
On this 30th anniversary, World AIDS Day gives us a time to pause and take in the enormity of this disease that has ravaged so much of humanity. There will be much written today about how we are turning a corner and that the epidemic is showing signs of coming to an end. It is important to celebrate and salute the great accomplishments in the fight against AIDS but it is also important to note that we are a long way from taking a victory lap. We do need to build momentum in the fight, so the accolades are helpful as long as they help generate enough buzz and enough energy to follow through by implementing and building on the advancements that have been made.
Unfair
The latest numbers show that there are about 34 Million people with HIV world-wide. At CFHI, because of our international partnerships, we are acutely aware that among all the world’s AIDS statistics it is particulary sobering to note that 60% of all cases are in Southern Africa and that South Africa has the horrible distinction of being the country with the most cases. Also it is important to note that statistics shoe that among all Asian countries, India has the most cases. When we look at global health disparities in general, we see how unfair the realities of burden of disease and access to healthcare are but in the context o this particular disease, it is somehow even more shocking. Try to take some time this World AIDS Day to educate yourself. The World Health organization has a wealth of information, you can start at this link.
One of the great privileges for me as part of CFHI, is the opportunity I get to visit doctors, nursers, and other healthcare workers in the field. As you really cannot even begin to imagine, communities where the prelevance of HIV/AIDS is very high, are impacted in a variety of ways. On World AIDS Day, I think back on the doctors and nurses in hospitals that are inundated with patients due to the epidemic yet they still push on, they still show up even when success is not a common part of their day. Finding local health professionals who are dedicated to their own underserved communities and trying to support them in their work is at the heart of what we do. We see them in hospital wards that are overflowing, we see them on strenuous trips to rural areas to test, educate, and treat -thus making treatment and healthcare accessible to more of the population. We see them in hospitals where the staff room has become a small ward or infection control area thus leaving them spending long hours working with no place to go for a break. We see them in clinics working tirelessly as as line of patients stretches out the door and down the street, more than a city block. We see them morn the loss not only of patients but of so many of their colleagues, and yet they continue. We see them in these situations every day, and we see them more dedicated and more earnest in their efforts each day. These are real heroes in this global fight and we salute you on this World AIDS Day and we pledge our continued efforts to help support and champion your work.
 On this World AIDS day, 2011, it is particularly wonderful to note that a new film is debuting in South Africa. Inside Story: the Science of HIV/AIDS will be premiering across South Africa. A wonderful attempt to target the exact population that the epidemic is targeting –young people. Using live action, computer animation and, yes, football (soccer), the goal is to educate through entertainment. Actors from different African countries are participating in hopes that the film will gain audiences across Africa. In addition to a love story and a sports story, the film shows through animation what is happening inside the body as HIV and AIDS run their course. The effort deserves a two thumbs up even though we have yet to actually see the whole film. We hope that this film can be more effective than any drug at combating the disease.
On this World AIDS day, 2011, it is particularly wonderful to note that a new film is debuting in South Africa. Inside Story: the Science of HIV/AIDS will be premiering across South Africa. A wonderful attempt to target the exact population that the epidemic is targeting –young people. Using live action, computer animation and, yes, football (soccer), the goal is to educate through entertainment. Actors from different African countries are participating in hopes that the film will gain audiences across Africa. In addition to a love story and a sports story, the film shows through animation what is happening inside the body as HIV and AIDS run their course. The effort deserves a two thumbs up even though we have yet to actually see the whole film. We hope that this film can be more effective than any drug at combating the disease.
CFHI’s Model for Global Health Electives Included in Oxford University Press Publication
“Global Health Ethics is once again in the forefront of discussion with the recently published Oxford Handbook of Neuroethics chapter emphasizing the relevance of biomedical, clinical and public health ethics within the global medical and academic community. Child Family Health International’s (CFHI) Evaleen Jones M.D., Jessica Evert M.D., Scott Loeliger M.D., and Steven Schmidbauer co-authored the chapter on the importance of establishing and sustaining an ethical framework for educational global health programs.
So reads the beginning of the Press Release for CFHI issued today. Needless to say, we are all very proud and very happy to have this recognition especially from such a noted publisher as Oxford University Press. The portion that CFHI contributed to this chapter on Global Health Ethics is an attempt to describe our model of working in underserved communities by identifying local experts and building on the inherent strengths of the communities. We have seen over and over again low-resource settings where amazing things are being accomplished every day in patient care due to extremely dedicated local professionals. We see their deep commitment to serving the people and we join together with the local health professionals to design Global Heath Education Programs that are open to international students and trainees. You can read our submission here but I want to take this opportunity to thank all our international partners who have chosen to work with us to develop this model and make it successful for the last 20 years. No partnership is one-sided and we are deeply indebted to all the local doctors and nurses, hospital and clinic staff, local coordinators, host families, language teachers, drivers and many others who make our international programs function so well, even in some very challenging circumstances. Our hats are off to all members of the CFHI global family –you all share in this recognition!
Read the full CFHI Press Relase and Chapter.
World Food Day
Today is World Food Day. The United Nations Food and Agriculture Organization has issued a report that should be on the ‘must read’ list of anyone interested in global health. There is some good news but also some disturbing news that should act as a wakeup call for the world community. Staple food prices are at or near all time highs. One of the most alarming facts in the report entitled Food Prices From Crisis to Stability is that just since last year the increases in the cost of basic food has, “pushed nearly 70 million people into extreme poverty.”
Past Successes Have Not Kept Pace
The report points out that while the world’s population doubled between 1960 and 2000, there were significant advances in agriculture that allowed food production to “meet and even exceed demand in many countries.” Unfortunately, the investments in research that were made, by both rich and poor countries, to produce the much needed innovations have not been maintained in recent decades. There has been a 43% decrease in government spending on research and development in the area of agriculture in the last 30 years. Therefore while the population of the world continues to increase, food production has not kept pace.
The last time food prices were this high was in 2008, when the price of various staple foods shot up very quickly and there was rioting in over 20 countries as a result. Certainly the global
economic situation is in even less shape to deal with record high food prices today. What’s worse is that due to the inability of food production to keep pace, “The global market is tight, with supply struggling to keep pace with demand and stocks are at or near historical lows.”
Promising New Successes
While the report warns that food price volatility may become an unsettling fact of life for the foreseeable future, it also gives some success stories that offer great hope. If we can prioritize research and development and scaling of existing successes, we may be able to prevent some of the volatility that now seems inevitable. Some scientific advances in Africa and Asia are resulting in higher yields but much more needs to be done in this area. Some countries have made increasing their food production a priority by encouraging agricultural land use and supporting research. Other countries like Mexico have been proactive in targeting assistance to some of the 70 million globally who are the new poor. Through carefully monitored programs tied to the education system, the Mexican government has been able to provide assistance to one in four families who have been hardest hit by rising food process. Even in these difficult times, this effort has, “…been credited with improving the health of children and adults, and raising nutrition and school enrollment levels.”
As we advocate for improved basic healthcare, we must also advocate for smart basic development that learns from the past and is doing the necessary research to keep up with our current and future needs. For the cornerstones of global public health continue to be water, food, sanitation, and education.
A Visit with The Father of Palliative Care in India
Dr. Rajagopal Dispenses Needed Medicines and a Healthy Dose of Respect.
After a meeting with CFHI’s Founder, Dr. Evaleen Jones at Stanford University, Dr. Rajagopal (Dr. Raj), the Founder of Pallium India agreed to become one of CFHI’s newest partners in India. CFHI India Coordinator, Ms. Hema Pandey, and I had the privilege of spending three days with him in Trivandrum, Southern India as we work to develop a CFHI Global Health Immersion Program exploring Palliative Care.
As the monsoon season takes its time to come to a close, the beautiful, lush countryside around Trivandrum in Kerala –Southern India is as calming as the  presence of Dr. Raj to his patients. We were given the great privilege of being allowed to shadow Dr. Raj during a day of home visits to various patients of Pallium India, the nonprofit he founded.
presence of Dr. Raj to his patients. We were given the great privilege of being allowed to shadow Dr. Raj during a day of home visits to various patients of Pallium India, the nonprofit he founded.
Who is Dr. Rajagopal
Dr. Raj is responsible for beginning the palliative care movement in India. He tells me that while the goal of palliative care might be the same in India as it is in England, where the modern hospice movement was started, the implementation is different. Dr. Raj feels that to simply pick up and transplant palliative care as it has been developed in the West can inadvertently have consequences that cause more suffering –when the main goal of palliative care is to reduce suffering. Dr, Raj is indeed a unique individual; he is both a visionary and a worker in the trenches. To follow him for a day doing home visits was inspiring. It was also a primer in how to do this kind of patient care.
Dr. Raj pointed out to me the four domains of patient care that were outlined by Cicely Saunders, the founder of the modern hospice movement. The four interlocking domains are Physical, Emotional, Social, and Spiritual. It is certainly a tall order for anyone to provide such comprehensive care, and to do it in low resource settings is even more challenging.
A Day in the Life– Implementing Palliative Care in India
As we drove into some of the poorest communities in Southern India, Dr. Raj and his team, a nurse, a social worker, and a driver went about their routine. Patient files are reviewed as we travel in the van. The size of the patient files is notable. After Dr. Raj read the file a bit, he begins to tell us the context of the family we are about to see. We get a succinct yet
thorough description of the family composition and history. The level of detail is impressive and we even had a few questions about the family that Dr. Raj answered from the record. I asked him when he last saw the family and he said that this was his first visit to them. There are three other teams conducting home visits and so the family has been seen by the other teams in the past. It is amazing to see the level of detail that is recorded from the home visit. From these notes, other services from nutrition, to physical therapy, to social work are provided –all driven initially from the teams’ weekly or fortnightly visits.
As we arrive, Dr. Raj gives warm and respectful greetings. He makes use of his reading of the chart right away to let the family know that he is up to speed on the situation even though this is his first time seeing them. Telling and retelling the story can be a help, at times, for a family but to have to do it with every healthcare worker that shows up, can become a burden.
In the home visit, Dr. Raj is totally in his element. Calm, positive, and respectful, he has a way of making the patient and the family feel that he has all the time in the world to spend with them –they have no idea that he has six more home visits to do. His careful touch, his undivided attention, his deep listening, his affirming comments are all the epitome of what a home visit should be. He listens and draws
out information to help him tweak the treatment plan based on what has happened since the previous home visit. As he leaves, he has given not only some medicines and ordered some more physical therapy but he has also given the family and the patient dignity, respect, and acknowledgment through his manner, his interactions, and his presence.
And, of course, as we make it back to the van, it’s time for Dr. Raj to write page after page of notes so the follow-up treatments can be done and so the next home visitor can pick up right where he left off.
CFHI Partners Develop Competency-Based Medical Education
What is Competency Based Education?
 Competency-based education (known as CBE) has been all the rage in medical education for nearly a decade. Competency in this realm has been described as the “habitual and judicious use of communication, knowledge, technical skills, clinical reasoning, emotions, values, and reflection in daily practice for the benefit of the individual and the community being served” Continue reading
Competency-based education (known as CBE) has been all the rage in medical education for nearly a decade. Competency in this realm has been described as the “habitual and judicious use of communication, knowledge, technical skills, clinical reasoning, emotions, values, and reflection in daily practice for the benefit of the individual and the community being served” Continue reading
CFHI Featured in Everyday Ambassador Blog
We at Child Family Health International (CFHI) are deeply honored to be featured in the Everyday Ambassador blog post by Kate Otto. Kate’s own accomplishments in global citizenship and smart diplomacy are considerable for anyone, especially for someone at such an early point in her career. She is a great example for students today who are interested in global service.
CFHI is equally proud to be a member of the International Volunteer Programs Association (IVPA), also featured in the blog post.
Many CFHI alumni are already doing their part in the Global Health field. With over 6,000 alumni now, we have a wonderful, growing family of everyday ambassadors who advocate and educate through their everyday activities. Through their first-hand accounts of shadowing local healthcare workers in underserved and low-resourced settings, they can speak with conviction and in compelling stories about the similarities and the differences of healthcare systems, and about important global health issues. Whether they do it in a professional capacity as a lecturer or professor, or in the informal setting of a party or a dinner, they can be equally effective in telling the story and enlightening people about global realities, thereby each doing his or her own part to bring us all closer together as the human family and improve the health of the world community.
You don’t have to be abroad to be making a difference. Visit our Facebook and LinkedIn pages and join in the conversations that are happening with people all around the globe. Follow #GlobalHealth on Twitter and keep yourself current on issues and causes. Share all of this with your own social networks and you will be surprised how much influence you can have as an individual. Our world is, in so many ways, becoming a ‘smaller place’. Be a part of it; participate!
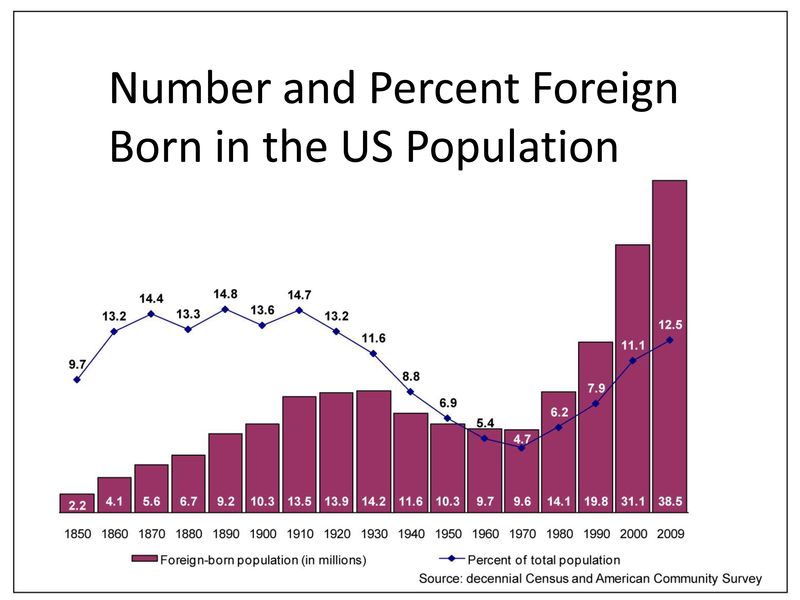
New US Census Data Shows Diversity of US Population Increasing
 “We are approaching a new highpoint in the prevalence of US residents who were born outside the country.” This is part of a message on the Director’s Blog of the US Census Bureau website that is aimed at the marketing industry, at advertisers of goods and services, but we at CFHI believe it is also important information for current and future health professionals.
“We are approaching a new highpoint in the prevalence of US residents who were born outside the country.” This is part of a message on the Director’s Blog of the US Census Bureau website that is aimed at the marketing industry, at advertisers of goods and services, but we at CFHI believe it is also important information for current and future health professionals.
While the Census Bureau is providing this new data, none of the basic trends of an increasingly diverse population for the United States should be a surprise to us. Forward thinking health professionals and medical educators have seen the indications of these trends for many years. Health science students (including medical students, nursing students, and public health students) have not waited for courses to be developed by the data that is now beginning to be analyzed, but have taken the initiative to seek out medical electives and rotations that would give them first-hand experience of different cultures and the different ways people view health around the world.
With some 6,000 alumni of CFHI Global Health Immersion Programs to date, we hear over and over again from them how their CFHI experience gave them insight into the role that culture plays in health and healthcare. Tenny Lee, a 2010 CFHI Mexico alum, reports: “My experience in Mexico has given my medical career a foundation to help underserved communities and break though language and cultural barriers.” You can read more about her CFHI experience in her review posted on the website Great Nonprofits. The ability to competently serve a more widely diverse patient population will clearly become the expectation for health professionals, as we can see from the wealth of information that the US Census Bureau is releasing.
 One of the most important data points released so far is that the Hispanic population of the US now exceeds 50 Million, a 43% increase since the last census as reported by CNN. And it is not just in border states in the south. The CNN article quotes demographer Jeffrey Passel at the Pew Hispanic Center as saying, “Previously, the Hispanic population was concentrated in eight or nine states; it is now spread throughout the country.”
One of the most important data points released so far is that the Hispanic population of the US now exceeds 50 Million, a 43% increase since the last census as reported by CNN. And it is not just in border states in the south. The CNN article quotes demographer Jeffrey Passel at the Pew Hispanic Center as saying, “Previously, the Hispanic population was concentrated in eight or nine states; it is now spread throughout the country.”
Medical schools, organizations, and institutions of higher learning have also recognized these trends, and CFHI has been happy to work with many of them to design specific programs. The Patient Advocacy Program at the Stanford Medical School began a program abroad with CFHI in 2007. The University of California at Davis has partnered with CHFI for over five years now to offer a Bi-National Health Quarter Abroad program for undergraduates in special arrangement with the Chicana/o Studies Department at UCD. Both of these programs also make use of CFHI’s built-in Spanish Language and Medical Spanish Instruction. Students are also living with host families so they are immersed into the culture during the program. Guided journaling and weekly meetings help students reflect and integrate what they are learning from their daily interactions. CFHI is also working with others, including Northwestern University, The Student National Medical Association (SNMA), -which you can read more about in an earlier posting– and the Public Health Institute in association with the Global Health Fellows Program. CFHI has been able to partner with each group and use our 20 years of experience working at the grassroots level in underserved communities abroad to design programs that meet specific learning objectives that are achieved in real life settings with the help of local health professionals who have the unique expertise of the local healthcare system and the best understanding of the local culture.
Jessica Brown, a 2010 CFHI Ecuador alum, pulls it all together in her reflection about her CFHI experience:
“… [I] learned a wealth of information about health that extended beyond the Reproductive realm.” Jessica goes on to say, “I learned a lot about Ecuador’s healthcare system by discussing health care access, education, socioeconomic class and ethnic background with my mentors and preceptors. I learned about how religion, education and customary social/cultural schools of thought (i.e. machismo) weigh heavily on Ecuador’s society, and individual minds; I saw how the cultural “way” dictated the population’s attitude towards healthcare, especially in Women’s Reproductive Health.
The moments that caused me to question belief systems in place within myself really stretched me beyond limits I never knew possible. And it is these reflections upon the state of health care in Quito that can broaden my understanding of client needs, beliefs and culture here in the states.”
Making Global Health Knowledge a Requirement for MD Students
A Post From CFHI’s Medical Director:
I’m just returning from conducting a workshop at the NEGEA Regional Conference. NEGEA is the Northeast educator’s chapter of the AAMC – a gathering of the people who oversee medical student and resident education. Just like many in global health medical education, they are grappling with how to get their hands around the subject and figure out how to increase collaboration.
Continue reading
CFHI Teams Up with SNMA for Special Global Health Experience
 CFHI and SNMA have teamed up to present this new and specialized program that offers participants the opportunity to participate in a 2-week global health program in the city of Oaxaca Mexico!
CFHI and SNMA have teamed up to present this new and specialized program that offers participants the opportunity to participate in a 2-week global health program in the city of Oaxaca Mexico!
The Student National Medical Association (SNMA) is the oldest and largest, student-run organization focused on the needs  and concerns of medical students of color. For over 40 years SNMA has been dedicated to ensuring culturally sensitive medical education and services. For 20 years, CFHI has been offering Global Health Immersion programs designed to help students appreciate the role that culture plays in health and healthcare. By teaming up, CFHI and SNMA hope to make a Global Health experience accessible to more students. This special 2-week program, previously open only to SNMA members, is now open to all health science students. Space is limited so apply early.
and concerns of medical students of color. For over 40 years SNMA has been dedicated to ensuring culturally sensitive medical education and services. For 20 years, CFHI has been offering Global Health Immersion programs designed to help students appreciate the role that culture plays in health and healthcare. By teaming up, CFHI and SNMA hope to make a Global Health experience accessible to more students. This special 2-week program, previously open only to SNMA members, is now open to all health science students. Space is limited so apply early.
The SNMA-CFHI 2-week Urban Primary Care in Oaxaca program aims to introduce students to the cultural competencies that are crucial for effective health care professionals. This program is tailored for those who wish to increase their cultural and linguistic competency as well as their understanding of the health factors affecting Latinos.
Oaxaca is an excellent setting for studying the healthcare system of Mexico and the healthcare practices of the population. Students often hold the false assumption that the healthcare is available to all, but find in Oaxaca that poor and rural populations are increasingly unable to compete for scarce health resources.
CFHI programs offer participants the opportunity to learn more about health issues that transcend national borders, class, ethnicity, and cultural divisions. By participating in CFHI’s global health education you will gain a unique insight into healthcare systems of developing countries and increase your cultural competency. Increasing one’s awareness of other cultures (cultural competency) is becoming increasingly relevant for healthcare professionals as industrialized countries become more ethnically, culturally and linguistically diverse. Click here to read an article and learn more about why cultural competency is important for today’s healthcare workforce.
The program dates are June 3rd to June 18th. Please visit the CFHI website to learn more.
We look forward to having you join our grassroots work to build a global community in support of better healthcare for underserved communities and more globally aware health professionals!
Familiarity That Melts Away Mistrust -Michelle Obama
As part of the official visit of President Hu to Washington, First Lady, Michelle Obama spoke to a captivated audience at Howard University saying that when you go abroad, “you are shaping the image of America projected to the rest of the world.” While Mrs. Obama was trying to promote a campaign to increase the number of students going to China, many of her comments are applicable to any cross cultural learning experience:
“…studying abroad isn’t just an important part of a well-rounded educational experience. It’s also becoming increasingly important for success in the modern global economy. Getting ahead in today’s workplaces isn’t just about the skills you bring from the classroom. It’s also about the experience you have with the world beyond our borders — with people, and languages, and cultures that are very different from our own.”
Last Spring, her husband, President Barack Obama, spoke to students at the University of Michigan saying: “As our world grows smaller, more connected. You will live and work with more people who don’t look like you, or think like you, or come from where you come from.” And almost in a response to these words by her husband, Mrs. Obama went on to say:
“That’s why it is so important for more of our young people to live and study in each other’s countries. That’s how, student by student, we develop that habit of cooperation, by immersing yourself in someone else’s culture, by sharing your stories and letting them share theirs, by taking the time to get past the stereotypes and misperceptions that too often divide us.
That’s how you build that familiarity that melts away mistrust. That’s how you begin to see yourselves in one another and realize how much we all share, no matter where we live. ”
CFHI programs have always focused on immersion into a culture, into a different helathcare system. Rather than staging impressive extraordinary displays for students, CHFI’s Global Health Immersion Programs give students a real slice of life, giving the participant and authentic experience of what it is like to be a health professional in that country. Some days may be very low key, other days in a hospital may be overwhelming. Regardless of the program, the bonds that students have made with professionals, with host families and with each other are very strong and lasting.
Global Health TV Looks at CFHI Program In India
 Global Health TV, based in London, recently visited one of CFHI’s Community Health Projects in India. The Catch Them Young Program is a health education program directed at youth ages 12-19 in a rural area outside the city of Pune. This is one example of a typical CFHI Community Health Project that originates at the local level and therefore has local ownership. CFHI has been happy to provide some of the funding to advance this project and to support the great dedication that local health professionals and community workers have to their own underserved communities.
Global Health TV, based in London, recently visited one of CFHI’s Community Health Projects in India. The Catch Them Young Program is a health education program directed at youth ages 12-19 in a rural area outside the city of Pune. This is one example of a typical CFHI Community Health Project that originates at the local level and therefore has local ownership. CFHI has been happy to provide some of the funding to advance this project and to support the great dedication that local health professionals and community workers have to their own underserved communities.
The 5 minute short film can be seen on the Global Health TV website. We have posted it to the CFHI YouTube Channel as well. It also shows one of CFHI’s Global Health Immersion Programs in India. CFHI seeks to identify local community health professionals who are dedicated to local underserved communities.
These unsung heroes are local experts and CFHI works with them to develop the 4-12 week Global Health Immersion Programs that international students of the health professions attend. The programs are empowering to the local community as the community sees their own health professionals instructing and mentoring international students. The film had its debut at the Canadian Conference on Global Health in Ottawa, November 1-3, 2010.
Report From Ottawa –The Canadian Global Health Conference
Global Health: a Humanitarian Crisis? With this urgent theme, the Canadian Society for International Health (CSIH) is holding its annual conference here in Ottawa.  Recognizing the progress and successes in the arena of Global Health, one of the messages of this conference is to not forget the crisis of the billions of people around the world living on less than $2.00 per day. With this reality, much of the focus here has been on issues of equity.
Recognizing the progress and successes in the arena of Global Health, one of the messages of this conference is to not forget the crisis of the billions of people around the world living on less than $2.00 per day. With this reality, much of the focus here has been on issues of equity.
While the sessions and sharing of ideas have been strong and fruitful, I have found a remarkable effort almost behind the scenes here to include and involve students in this professional conference. I have had the opportunity this year to speak with students in Australia, the UK, the US, and now here in Canada and in all places the interest in Global Health is continuing to grow. Everywhere I go, I find students looking for career paths and guidance in the field of Global Health. Here in Ottawa, I have seen a level of inclusion, mentoring, and respect for students that I have never seen before. Students from across Canada are here with financial and moral support from their schools and students themselves are engaged with the academic world as well as the professional world. Students are taken seriously here and they are responding and rising to that expectation. It is a lesson for Global Health educators around the world to heed.
The leadership of CSIH, as well as the national academic leaders are setting the example by intentionally engaging in efforts to cultivate, nurture and mentor the Global Health professionals of the future not just in the classroom, and not just though international trips but in their own offices and their daily work. Because they are truly engaging and listening to the students, educators are also able to take the appropriate next steps to advance Global Health education and not just marvel at the surge in student interest. Great work has been done on a set of Global Health Core Competencies that can serve as a much needed foundation for faculty and students alike.
CFHI Alum Reflects on Her Experience in South Africa
Stella Chiu who spent part of her summer on one of CFHI’s Global Health Immersion Programs in South Africa contributed to a blog on the IE3 Global Internships website. Her blog post Coming Home with New Perspectives is an honest sharing of her thoughts as she is still in the re-entry process. Stella says, “I haven’t had any major problems re-integrating. However, the only difficulties I’ve encountered are through the new perspectives that I’ve gained.”
Coming Home with New Perspectives is an honest sharing of her thoughts as she is still in the re-entry process. Stella says, “I haven’t had any major problems re-integrating. However, the only difficulties I’ve encountered are through the new perspectives that I’ve gained.”
Stella reports that after being completely immersed in the South African culture and healthcare system, and especially with the warm welcome of her South African host family, she now finds herself, at times, ‘homesick’ for South Africa. Stella recommends to others who go abroad to build in time to reflect after coming home, to “sit down and think” so that you can become aware of how your perspective has changed “both personally and professionally” by what you have experienced. She says of her friends, “Sometimes it is hard for others to understand my outlook on certain things because they have not experienced what I have experienced.”
As part of her own reflection, Stella shares, “I am grateful for the opportunity CHFI-South Africa has given me in developing my clinical skills and finding my niche. I did rotations in surgery, pediatrics, ophthalmology, and in internal medicine and found an unexpected love for surgery. I grew to understand South Africa’s health care system, as well as its deficiencies, setting the groundwork for when I can return someday to work. I have built lifelong relationships with students in the program, and the families that I stayed with. I know that I will always have a home in South Africa.”
We wish Stella well as she continues her re-entry and we know that her host family and those who worked with her in South Africa were grateful for her presence and will never forget her.
Open Education Resources for Global Health Education
Here is a follow-up By Dr. Jessica Evert, CFHI Medical Director, from the CUGH Conference, see earlier posts from Sept 20th and Sept 21st.
I am excited about the open access movement, in publishing, medical education, and in global health. The prospect of Open Educational Resources (OER) in addressing workforce issues and the education drought in many low resource countries is quite promising. Tufts and University of Michigan presented there work in this area at  the recent CUGH meeting in Seattle, Washington. Erica Frank, who recently moved from Emory to UBC, also presented on her Health Sciences Online project which provides over 50,000 educational resources in over 40 languages (it is powered by Google Translator), that are not only free, but ad-free. Perhaps the most inspiring presentation was by Richard Adanu, from University of Ghana, who presented on OERAfrica. His step-by-step instruction for a cesarean section can be found at this link. He commented on a unique issue at teaching hospitals in Ghana, and many places in Africa. Unlike in the US where there are one or two students in each surgical procedure trying to learn, in Ghana there may be ten or even more. Thus, it is almost impossible for the students to see the procedure. These videos help immensely so students can actually see the procedure. One of my concerns about exporting US medical school curriculum to Africa or other places is that it might not be applicable. I asked Dr. Adanu about this issue. He said that while there may be certain things that are different (the brand of medication available, or specific cultural acceptance of interventions), generally these online resources are viewed before class by students, and then serve as the focal point of a conversation in the classroom setting, where instructors can discuss the local variations and context. Interestingly, Tufts is using their open source software called TUSK to allow medical schools abroad to customize curriculum and utilize smart phone technology to tele-consult and have other collaborative discussions. One faculty member in the audiences commented that in ten years this may put teaching faculty out of business. A panelist replied that it will require that teaches become facilitators of discussions and critical thinking, rather than merely deliverers of information. Half joking, but maybe actually not, moderator David Stern commented, “in the future we may get promoted based on the number of hits we get.” This is a real possibility- any maybe hits from sub-Saharan Africa and low resource countries should carry extra weight in the promotional review. Have you utilized Open Educational Resources (OER)? Feel free to share your experience.
the recent CUGH meeting in Seattle, Washington. Erica Frank, who recently moved from Emory to UBC, also presented on her Health Sciences Online project which provides over 50,000 educational resources in over 40 languages (it is powered by Google Translator), that are not only free, but ad-free. Perhaps the most inspiring presentation was by Richard Adanu, from University of Ghana, who presented on OERAfrica. His step-by-step instruction for a cesarean section can be found at this link. He commented on a unique issue at teaching hospitals in Ghana, and many places in Africa. Unlike in the US where there are one or two students in each surgical procedure trying to learn, in Ghana there may be ten or even more. Thus, it is almost impossible for the students to see the procedure. These videos help immensely so students can actually see the procedure. One of my concerns about exporting US medical school curriculum to Africa or other places is that it might not be applicable. I asked Dr. Adanu about this issue. He said that while there may be certain things that are different (the brand of medication available, or specific cultural acceptance of interventions), generally these online resources are viewed before class by students, and then serve as the focal point of a conversation in the classroom setting, where instructors can discuss the local variations and context. Interestingly, Tufts is using their open source software called TUSK to allow medical schools abroad to customize curriculum and utilize smart phone technology to tele-consult and have other collaborative discussions. One faculty member in the audiences commented that in ten years this may put teaching faculty out of business. A panelist replied that it will require that teaches become facilitators of discussions and critical thinking, rather than merely deliverers of information. Half joking, but maybe actually not, moderator David Stern commented, “in the future we may get promoted based on the number of hits we get.” This is a real possibility- any maybe hits from sub-Saharan Africa and low resource countries should carry extra weight in the promotional review. Have you utilized Open Educational Resources (OER)? Feel free to share your experience.
CFHI Medical Director Blogs on Day 2 of CUGH Conference
This is the second of two guest blogs by Jessica Evert, MD, CFHI Medical Director, blogging from the CUGH Annual Meeting in Seattle. Be sure to leave a comment.
Ann Dower of University of Washington’s I-TECH Center said today “we must practice the art of partnership” in order to be successful in global health. Additionally, I was struck when Kevin De Cock MD, Director of the Center for Global Health at CDC, candidly reflected on his early career immersion experience in Nairobi, Kenya, saying, “I wish I was more humble.” I think this humility and the ability to form meaningful partnerships go hand-in-hand.
This idea of ‘partnership’ has come up countless times at the CUGH meeting over the last 2 days. Many seasoned global health experts have lamented over the lack of partnerships and failures of global health attempts due to this shortcoming. How can we learn from this history? How can we build training and educational programs that prioritize partnership? It seems that many times our process (the process of US based individuals, universities, and organizations) of global engagement is not necessarily the best approach to foster partnership or humility. We often have our own ideas of how to solve problems based on our views and our skills, rather than based on the voice of communities abroad. In academia, there is the nagging issue of faculty, and sometimes students, having to demonstrate personal accomplishments and quick outcomes which often trump the empowerment of communities to own the accomplishments and guide the outcomes. To find the answer to these important questions we need to look at how we frame introductory global health experiences for health science trainees (pre-health, medical, nursing, public health, allied health, dental, and other students) and how our academic institutions approach global engagement. The first experience abroad (a stepping stone experience) or first visit to a region or country is pivotal to frame how future global engagement occurs. If individuals go abroad and set-up a tent clinic outside the local healthcare infrastructure, an appreciation for local capacity, systems, and workforce is not realized. If students go to a hospital with faculty from their US institution who displace local physicians and assumes US clinical expertise translates immediately into similar expertise in an international setting, the student sees the glorification of US faculty, rather than the appreciation of unique practices, language, and expertise of local, native practitioners. It is time we recognize that the skills necessary for partnership need to be fostered from early levels of engagement and need to be modeled by our US teaching institutions and mentors.
How do we teach health science students and trainees about partnerships? What skills does partnership require? To delve into these questions, we must define partnership. The Partnering Initiative, an NGO that specializes in partnership training, defines partnership as follows: “a cross-sector collaboration in which organisations work together in a transparent, equitable and mutually beneficial way towards a sustainable development goal and where those defined as partners agree to commit resources and share the risks as well as the benefits associated with the partnership.” This is no simple task. They also define the partnering principles as follows- equity, transparency, mutual benefit. If partnership is fundamental to the success of global health activities, then we must judge global health activities in part based on these fundamental principles. The need for trust, mutual respect, and communication are presupposed in the process of building partnerships.
We can teach the principles and precursors to partnership through thoughtful global health immersion programs. I am proud to be a part of CFHI. I think CFHI is setting a standard for both academic and NGO based immersion programs. I liken CFHI immersion programs to participant-observation techniques I utilized during my thesis work. In anthropology the mechanism of understanding a culture, community, and executing research is participant-observation. Participant observation involves gaining an understanding of another social group or community, by inserting yourself into that community in a way that is agreeable to the community, while observing the practices and learning about the culture, social structure, systems, and other behaviors. CFHI immersion experiences provide an opportunity for participant-observation. I would argue that such participant-observation, done in the context of long-term CFHI partnerships, lay the groundwork and start fostering skills necessary to form meaningful partnerships with individuals and organizations abroad. The local health care providers are the experts who teach CFHI participants what their communities are facing. We have received feedback from partners that patients consider their local providers more capable because they are teaching western health science students (rather than Western physicians or students providing the expertise in patient care at the international setting). This dynamic is very important and very powerful. The first step in the cycle of partnership, as defined by The Partnering Institute, is “scoping.” In essence we are teaching our students and trainees how to scope, which includes listening, observing, and appreciating a local reality before trying to change it.
If partnerships are key to the success of global health programs and interventions, it is time we look at what it takes to impart the skills necessary to foster partnerships. These skills include observation, humility, and restraint so we can give voice to the local community and engage in truly mutually beneficial ways. By providing stepping stone global health immersion programs that prioritize the “scoping” necessary to form partnerships, we can engender a new generation of globally-active professionals who understand from early in their exposure and interaction with global communities the fundamentals of partnership and humility that Dr. De Cook and others wish they knew from the start. It reminds me of a quote by Nietzche, “When one has finished building one’s house, one suddenly realizes that in the process one has learned something that one really needed to know in the worst way – before one began.” We can provide these lessons before students build their proverbial global health houses through conscientious global health immersion.
Observations From CUGH’s Annual Meeting
What follows is a Guest Blog by Jessica Evert, MD, CFHI Medical Director, who is attending the CUGH Annual Meeting in Seattle. Previous entries with Jessica are here and here
The opening plenary of CUGH’s Second Annual Meeting (Consortium of Universities in Global Health) was marked by discussion of the great successes and challenges in global health. A live feed from TEDxChange, a non-profit dedicated to the exploring ideas and giving space to innovative thinkers, opened the morning with inspirational data presented by Hans Rosling and commentary by Melinda Gates. The conclusion by Rosling was that there is no “developing” and “developed” world; he cited the fact that countries with some of the best indicators of child survival and birthrate are still considered “developing.” He also gave a very positive report on the progress toward MDGs, specifically reduction of poverty. He emphasized that we cannot consider Africa to be homogeneous, whereas, places such as the Congo have been stagnant on indicators such as child mortality, countries like Kenya have made great strides. Interestingly, Rosling overlaid a graph of the progress by Sweden over the last 200 years, which demonstrated their slow progress in the area of child mortality (400/1000 in 1800) in the first 100 of those years. This was powerful to give a long-term view of the progress that has only been started in the context of the last 10 years of the MDG campaign.
Melinda Gates utilized the model of Coca-Cola in their ability to penetrate far-reaching communities in the world (over 1.5 billion cokes are consumed a day) and promote their product in a positive light (a current marketing slogan being “Open Happiness”). One of the components of this success is the appreciation of and capitalization on local entrepreneurs. I liken this to the importance of local health professionals in global health goals and programs. Gates pointed out that our health improvement or preservation messages are often in a negative light- ‘avoid disease,’ ‘combat germs,’ ‘control infection.’ Rather, she purports, that if we utilize positive messages that draw on popular culture methods (hip hop, fashion, celebrations) it will be more effective. She encourages us to “look at what people want” and market health interventions to those aspirations.
Subsequently a panel of speakers made comments about global health and the role of universities. A common theme is the role of “collaboration” and “developing relationships.”  They universally endorsed the importance of international experiences for trainees. During the Q & A session I brought to the attention of the audience and panel that US medical schools, almost universally, do not require global health education for medical students. In addition, global health is not a topic on the medical school boards. In my opinion, a catalyst for the adoption of global health topics as part of the required medical school curriculum in the US is the inclusion of global health topics in the medical school board exams. We can draw on the experience of preventive medicine/public health, which were recent categorical additions to the medical school boards. This proposition begs a question, which is not an easy one, and was put to me by King Holmes after the session, “what do we add?” Yes, global health is a broad field, and yes, narrowing that down to curriculum that is digestible by US medical schools is a challenge. However, there are multiple organizations and individuals who are grappling with these questions- including the Global Health Education Consortium (GHEC). To let the broad scope of ‘global health’ be our barrier or excuse for not integrating it into US medical school education is to succumb to the most basic cop-out that deters many from working toward the most basic, yet overwhelming, challenges to health at home and abroad- including equity, access, compliance, and the like.
They universally endorsed the importance of international experiences for trainees. During the Q & A session I brought to the attention of the audience and panel that US medical schools, almost universally, do not require global health education for medical students. In addition, global health is not a topic on the medical school boards. In my opinion, a catalyst for the adoption of global health topics as part of the required medical school curriculum in the US is the inclusion of global health topics in the medical school board exams. We can draw on the experience of preventive medicine/public health, which were recent categorical additions to the medical school boards. This proposition begs a question, which is not an easy one, and was put to me by King Holmes after the session, “what do we add?” Yes, global health is a broad field, and yes, narrowing that down to curriculum that is digestible by US medical schools is a challenge. However, there are multiple organizations and individuals who are grappling with these questions- including the Global Health Education Consortium (GHEC). To let the broad scope of ‘global health’ be our barrier or excuse for not integrating it into US medical school education is to succumb to the most basic cop-out that deters many from working toward the most basic, yet overwhelming, challenges to health at home and abroad- including equity, access, compliance, and the like.
I encourage the global health education community, and the larger global health university movement, which is embodied by CUGH, to look in their own backyards, medical/nursing/allied health schools and wider university programs to embrace global health curriculum in a real way. In many US medical schools, students are begging for global health education, exposure, and experiences. To adopt required global health topics into the medical school curriculums is a basic step which these universities have control over. A manageable curriculum could include: basic lessons on the global burden of disease (including infectious disease, mental health, maternal/child mortality, and chronic disease), overview of global health initiatives (such as MDGs, PEPFAR, Global Fund), and discussions of inequities (as evidenced by the 10/90 gap, health disparities). The next question is who teaches these issues- at many of the larger, well-funded universities, experts may be internal and easily accessible. However, there is a challenge at many, even large, medical schools, who lack faculty with expertise in global health. This is where the role of non-profits and global health educational organizations is essential. Schools can utilize resources such as the global health education modules created by Global Health Education Consortium which bring experts to the classroom through PowerPoint presentations with evaluation. Also, many communities have non-profits or church-based organizations who are active globally. Engaging in global health activities does not necessarily correlate with the ability to teach basic global health education, however, we must start somewhere.Unlike cardiology, endocrinology, and other themes taught in medical school, global health is not a cookie-cutter experience or topic. However, if CUGH and organizations, such as the AAMC, require US medical schools to teach basic global health lessons to all medical students, and elevate the importance of these topics, medical schools will be given a tangible requirement that they can respond to with curriculum and faculty development.
Finally, I was struck by the university leaders’ agreement that ‘relationship building’ and ‘collaboration’ are necessary for any global health endeavor to be successful. Our medical schools have great challenges in building these relationships because of unreliable funding streams, focus on outcomes and accomplishments (often at the expense of an appreciation of process and community involvement), and staff/faculty turnover. There is also an inflexibility that is prominent in medical schools and institutions where state department advisories can lead to the complete withdrawal from a country, leaving partners to consider us ‘fair weather friends,’ and there is a tendency for wanting partnerships to fit into a programmatic mold. I hope the university community will see the benefit of partnerships with non-profit organizations, such as CFHI, who have the flexibility, continuity of staff/mission, and reliable funding streams to help facilitate international experiences for trainees in a fashion that is ethically, fiscally, and culturally sound.
CUGH is making their debut in many ways over the coming couple of days. I hope that their ability to leverage universities in the US will lead to increased global health exposure of our health science trainees, so that we are truly training the globally minded professionals that the future requires. In addition, I hope that momentum at the university level recognizes the role of non-governmental (and often not primarily academic) organizations who are setting standards in community engagement and training future health care providers in a way that elevates international communities as the ‘experts’ of their own environment that they are.
CFHI Alum: “It Made Me Want To Be A Doctor A Lot More…”
“It made me want to be a doctor a lot more, for sure,” she said. “Seeing doctors in action, they were really fantastic role models. It’s hard to get exposure shadowing doctors here (in the Bay Area). I’ve had a few opportunities at Stanford. The more time I got… the more inspired I am to become a doctor.” These are the words of Christina O’Neal, as reported in the Contra Costa Times by Correspondent Doug Mead. Christina, a Stanford University premedical student, spent part of her summer in the Cultural Crossroads in Health Program in  Oaxaca, Mexico.
Oaxaca, Mexico.
Christina told the Contra Costa Times in the article that her month on the CFHI program in Oaxaca, “was pretty life-changing. Everybody gets pretty much free health care there,” she said. “It’s interesting to see how things are run. There’s a lot of poverty, and the government, in terms of health care, has a lot of problems. But the infrastructure was good. I was impressed with how smooth it ran and how dedicated the doctors were. It was an awesome experience.”
The experience really improved Christina’s Spanish and Medical Spanish skills. “I’d say, before I got there, I was conversational (in Spanish),” she said. “Now, I’m borderline fluent. My comprehension, especially, skyrocketed. I’ve always had a pretty standard ability to speak. Now, I understand everything that’s happening. Even though my vocabulary didn’t grow as much, I can express myself better. Once you understand people better, it helps you to speak more correctly. We went over grammar and medical vocabulary every day (in class).”
We are very glad for Christina that her experience was so impactful and we greatly appreciate her kind words about the CFHI program as she ended her interview with the newspaper saying, “Everything was fantastic. It surpassed all my expectations. It was a phenomenal experience.”